
5 Safe & Natural Hyperhidrosis Solutions
Searching for natural hyperhidrosis solutions? Explore 5 safe ways to tackle excessive sweating and see why The Fischer Iontophoresis Device is the standout option.

Packet for physicians to complete for patients wishing to file for insurance coverage of the Fischer iontophoresis device.

Authorization form for the PureWick™ Urine Collection System.

Benohanian, Boudjikanian & Paylan [2007]

Gordon & Hill [2013]

McConaghy [2018]

Stolman [1987]
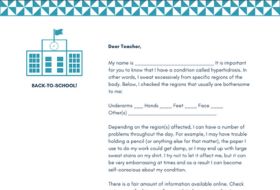
A letter for students to take to school that helps explains their symptoms to teachers and faculty.

A poster for your office that explains hyperhidrosis for patients.

A poster for your office with the different options for treating excessive sweating.

Our extended medical necessity letter provides a detailed rationale for insurance coverage of an iontophoresis device, highlighting its importance in treating hyperhidrosis effectively.
![Picture of a patient discussing something with his significant other, holding a pad of paper, dressed professionally [insurance coverage for medical supplies] [ Personalized urology care ]](https://www.rafischer.com/wp-content/uploads/2023/09/ra-fischer-home-medical-supply-iontophoresis-hyperhidrosis-conditions-cancer-neurogenic-bladder-urinary-retention-patient-success-doctor-referral-insurance-6.webp)




![Side view photograph showcasing the white, rectangular 'main control unit' of RA Fischer's 'The Fischer' Device - an iontophoresis device meticulously tailored for hyperhidrosis (excessive sweating) treatment.. The image features a white background [ Iontophoresis Device for Sweating ]](https://www.rafischer.com/wp-content/uploads/2023/09/the-fischer-iontophoresis-machine-hyperhidrosis-sweat-treatment-home-hospital-insurance-fda-approved-ra-fischer-14-scaled.webp)
![Image highlighting the back panel of RA Fischer's 'The Fischer' Device, showcasing the white, rectangular 'main control unit.' This specialized iontophoresis device is specifically designed to address hyperhidrosis (excessive sweating). In the photograph, you can discern the power switch and the electrode ports. The background is solid white. [ Iontophoresis Device for Sweating ]](https://www.rafischer.com/wp-content/uploads/2023/09/the-fischer-iontophoresis-machine-hyperhidrosis-sweat-treatment-home-hospital-insurance-fda-approved-ra-fischer-11-scaled.webp)
![Detailed image showcasing the black, metal-free silicone electrodes designed for RA Fischer's iontophoresis device, 'The Fischer,' used in the treatment of hyperhidrosis. The background is plain white. [ Iontophoresis Device for Sweating ]](https://www.rafischer.com/wp-content/uploads/2023/09/the-fischer-iontophoresis-machine-hyperhidrosis-sweat-treatment-home-hospital-insurance-fda-approved-ra-fischer-22-scaled.webp)

![Photograph that precisely spotlights one of the white water bath trays and the black, metal-free silicone electrode contained within RA Fischer's 'The Fischer' Device—an iontophoresis device meticulously designed for the treatment of hyperhidrosis (excessive sweating). The electrode is positioned inside the tray, and the entire composition is set against a clean white background. [ Iontophoresis Device for Sweating ]](https://www.rafischer.com/wp-content/uploads/2023/09/the-fischer-iontophoresis-machine-hyperhidrosis-sweat-treatment-home-hospital-insurance-fda-approved-ra-fischer-16-scaled.webp)
![Close-up photograph with a specific focus on one of the white water bath trays and the black, metal-free silicone electrodes integrated into RA Fischer's 'The Fischer' iontophoresis device; an iontophoresis device designed for the treatment of hyperhidrosis (excessive sweating). The trays feature blue pH-balancing foam and black metal-free silicone electrodes, all presented against a clean white background. [ Iontophoresis Device for Sweating ]](https://www.rafischer.com/wp-content/uploads/2023/09/the-fischer-iontophoresis-machine-hyperhidrosis-sweat-treatment-home-hospital-insurance-fda-approved-ra-fischer-17-scaled.webp)
![Detailed close-up image highlighting one of the white water bath trays and the black, metal-free silicone electrodes integrated into RA Fischer's 'The Fischer' Device—an iontophoresis device utilized for the treatment of hyperhidrosis (excessive sweating). The trays feature ph-balancing foam and metal-free silicone electrodes, all against a clean white background. [ Iontophoresis Device for Sweating ]](https://www.rafischer.com/wp-content/uploads/2023/09/the-fischer-iontophoresis-machine-hyperhidrosis-sweat-treatment-home-hospital-insurance-fda-approved-ra-fischer-20-scaled.webp)
![An up-close picture that focuses on the white water bath trays and the black, metal-free silicone electrodes incorporated within RA Fischer's 'The Fischer' Device. The trays include ph-balancing foam and metal-free silicone electrodes, presented against a clean white background. Iontophoresis device used for the treatment of hyperhidrosis (excessive sweating) [ Iontophoresis Device for Sweating ]](https://www.rafischer.com/wp-content/uploads/2023/09/the-fischer-iontophoresis-machine-hyperhidrosis-sweat-treatment-home-hospital-insurance-fda-approved-ra-fischer-21-scaled.webp)



![A detailed photograph featuring the metal-free silicone underarm attachments of RA Fischer's 'The Fischer' Device—an iontophoresis device intricately designed for the treatment of hyperhidrosis (excessive sweating). These attachments contain small black electrodes enclosed within white, textile-like sleeves. Their purpose is specifically geared toward the management of axillary (underarm) hyperhidrosis. [ Iontophoresis Device for Sweating ]](https://www.rafischer.com/wp-content/uploads/2023/09/the-fischer-iontophoresis-machine-hyperhidrosis-sweat-treatment-home-hospital-insurance-fda-approved-ra-fischer-7-scaled.webp)


Searching for natural hyperhidrosis solutions? Explore 5 safe ways to tackle excessive sweating and see why The Fischer Iontophoresis Device is the standout option.

Discover how scheduling a telehealth consultation through trusted partners like HubMD, CallOnDoc, and SkyMD can provide fast, expert care for a variety of conditions.

Wondering whether direct or pulsed current iontophoresis is better? Learn the differences, advantages, and how The Fischer combines both for optimal hyperhidrosis treatment.

Wondering why you’re sweating “there”? Discover the answers to essential hyperhidrosis questions, including symptoms, types, and effective treatments like iontophoresis.